DBC’s Op-ed in The Hill Times

Canadians deserve the best science to guide their cancer care. Let’s hope the government gives us that.
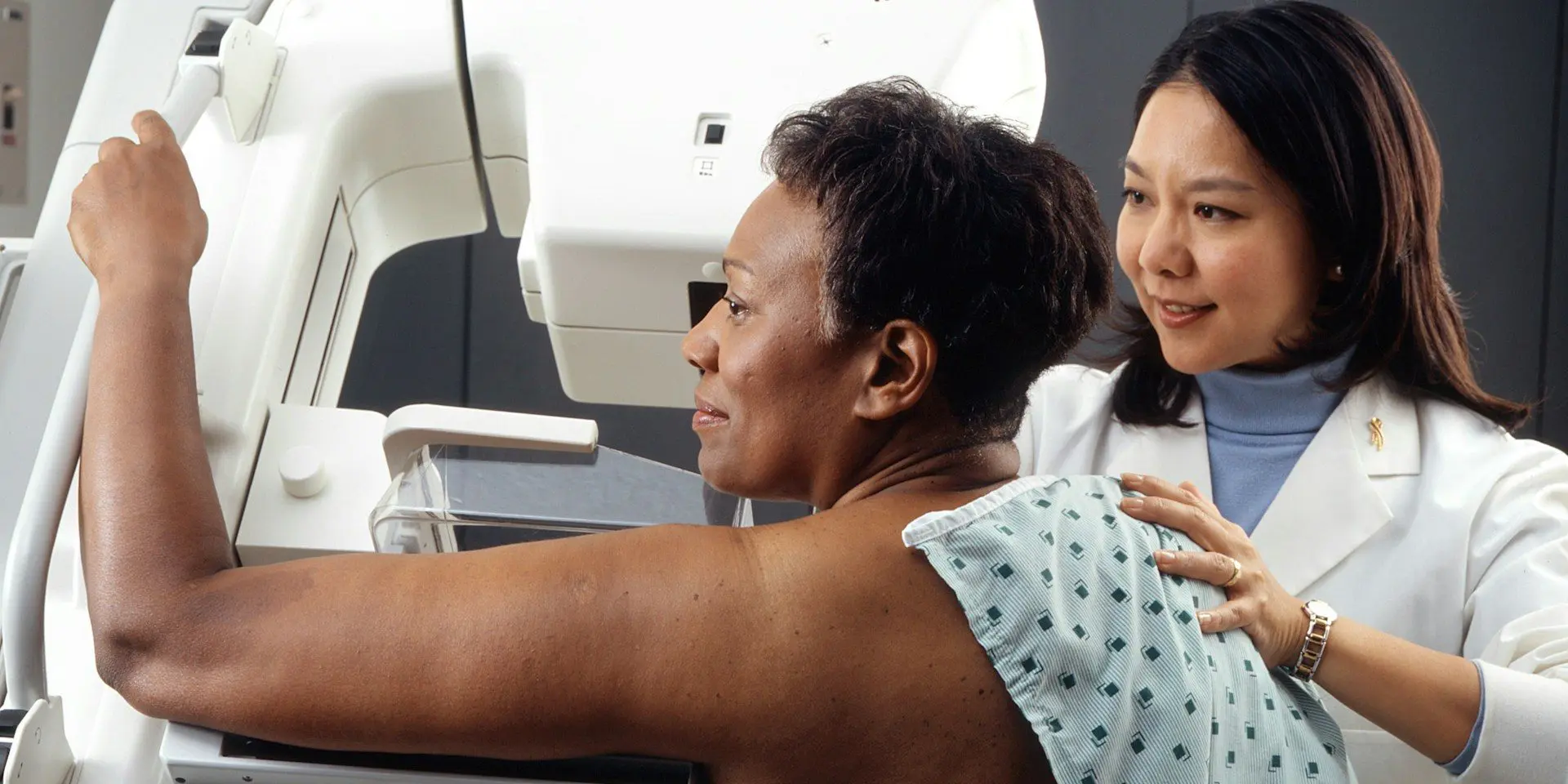
On this World Cancer Day, Canadians are hoping our government gives them the best chance at surviving this terrible disease. We hope that our government embraces the best science for protecting our health.
But cancer patients like me, cancer care experts, and researchers are worried that may not happen.

The Canadian Task Force on Preventive Health Care is the body which governs screening guidelines for cancer and other critical diseases. When the federal government paused the work of the task force and launched an external expert review panel last year, many clinicians and researchers welcomed the move. It was widely seen as an acknowledgment of long-standing concerns about how the task force was operating: narrow approaches to evidence, sidelining of advice from subject-matter experts, and guideline recommendations that often lacked clinical credibility.
The promise of reform raised expectations. The new task force will begin in April.
I am among a group of people provided with an early draft of the government’s plans for that group. Regrettably, those plans show that a central problem remains unresolved: subject-matter experts, those with scientific and clinical expertise in the diseases under review, are still not meaningfully embedded in either evidence synthesis or guideline decision-making. Current conflict-of-interest guidelines are so restrictive that they systematically exclude virtually all legitimate subject-matter experts.
This is not a minor procedural issue. It is a foundational flaw.
High-quality guidelines depend on both methodological rigour and clinical relevance. Evidence to support guidelines is created by evidence synthesis teams composed of skilled methodologists. Both the evidence review teams and the task force must include subject matter experts to determine how evidence should be framed, interpreted, or applied, especially in complex, evolving fields such as cancer screening. If subject-matter experts are absent or consulted only superficially, then the risk of misinterpretation is baked in from start to finish.
When expert involvement is performative rather than substantive, guideline quality suffers and trust erodes.
This is not an unsolved problem. European guideline systems demonstrate that rigour and expertise are not competing values, but complementary ones.
Bodies such as the European Commission Initiative on Breast Cancer and the European Society of Breast Imaging explicitly embed radiologists and other disease-specific experts into multidisciplinary panels that oversee both evidence synthesis and guideline development. Observational data, registry evidence, and real-world outcomes are formally considered, with expert judgment documented rather than suppressed.
In these systems, clinical expertise is not treated as a conflict to be excluded. It is treated as a safeguard against misinterpretation.
The contrast with the current plans for Canada is stark. A model that restricts expert participation to advisory roles or excludes it entirely at key decision points cannot credibly claim to meet the best standards.
Reform must address structure. At a minimum, meaningful modernization would require:
- Mandated inclusion of subject-matter experts on evidence synthesis teams from the outset of each guideline project;
- A standing, transparent roster of experts across relevant disease areas, developed with input from specialty colleges and professional associations;
- Roles for experts that are genuinely influential, either as voting members in evidence synthesis and guideline development, or through a permanent Subject-Matter Experts Committee whose endorsement is required for guideline approval; and
- Robust conflict-of-interest management that distinguishes expertise from bias, rather than using conflict frameworks to exclude knowledge.
These approaches are neither radical nor untested. They are standard features of many credible scientific and regulatory processes worldwide.
Guideline reform that preserves methodological rigidity while continuing to sideline subject-matter experts will not restore confidence or improve outcomes. It will perpetuate the very problems that led to the Task Force pause in the first place.
If Canada is serious about protecting public trust and improving cancer outcomes, it must stop treating expertise as a liability and start recognizing it as essential.
Jennie Dale is the co-founder and executive director of Dense Breasts Canada, a volunteer run, non-profit founded in 2016.
The Hill Times











